Case Series/Study
(CS-009) Stimulation of Perfusion and Healing Using Microvascular Tissue in a Series of Refractory Complex Diabetic Wound Cases
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Introduction: Structural microvascular tissue allograft (PMVT*) has previously demonstrated increased healing and wound perfusion in a 100-subject randomized controlled trial on Wagner 1/2 DFUs.1 PMVT’s microvascular extracellular matrix composition drives host cell attachment and supports angiogenesis, important modes of action in the treatment of wounds with deficient microvascular tissue.2 Here we report on real-world clinical experiences with PMVT in three challenging nonhealing wounds.
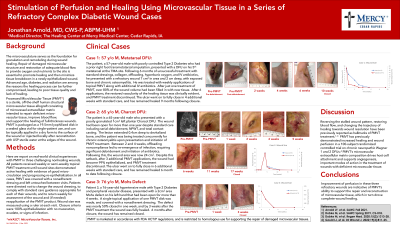
Methods: Patient 1 was a 57-year-old male with a prior right foot transmetatarsal amputation (TMA) who developed a DFU on his 5th metatarsal at the TMA site. Following six months of unsuccessful treatment with standard dressings, collagen, offloading, hyperbaric oxygen, and IV antibiotics, he presented with a refractory wound 7cm2 in area and 2cm deep with exposed bone and chronic osteomyelitis, and was treated with PMVT along with additional IV antibiotics. Patient 2, a 65-year-old male, presented with a poorly granulated 1cm2 left plantar Charcot DFU open for more than one year despite standard care including serial debridement, NPWT, and total contact casting. The lesion extended 0.4cm to devitalized bone, and the patient was being treated concurrently for chronic osteomyelitis upon initiation of PMVT treatment. Patient 3 was a 76-year-old hypertensive male with peripheral vascular disease who presented with a 2cm2 area Mohs defect on his left hand. All patients received weekly topical PMVT treatment until wound sites demonstrated active healing with evidence of good microcirculation and progressing re-epithelialization.
Results: The patients required 6, 7, and 1 topical mVASC applications, respectively, at which point restored vascularity of the healing tissue was clinically evident, and PMVT treatment discontinued. In all three cases the wounds fully healed within several weeks after completing PMVT application. Patients have been followed one to four months after healing, and all wounds remain closed.
Discussion: Reversing the stalled wound pattern and changing the trajectory of healing towards wound resolution has been previously reported as a hallmark of PMVT treatment.3,4 Improvement of perfusion in these three refractory diabetic wounds are indicative of PMVT’s ability to support the repair and reconstruction of microvascular tissue, which in turn drove complete wound healing.
Methods: Patient 1 was a 57-year-old male with a prior right foot transmetatarsal amputation (TMA) who developed a DFU on his 5th metatarsal at the TMA site. Following six months of unsuccessful treatment with standard dressings, collagen, offloading, hyperbaric oxygen, and IV antibiotics, he presented with a refractory wound 7cm2 in area and 2cm deep with exposed bone and chronic osteomyelitis, and was treated with PMVT along with additional IV antibiotics. Patient 2, a 65-year-old male, presented with a poorly granulated 1cm2 left plantar Charcot DFU open for more than one year despite standard care including serial debridement, NPWT, and total contact casting. The lesion extended 0.4cm to devitalized bone, and the patient was being treated concurrently for chronic osteomyelitis upon initiation of PMVT treatment. Patient 3 was a 76-year-old hypertensive male with peripheral vascular disease who presented with a 2cm2 area Mohs defect on his left hand. All patients received weekly topical PMVT treatment until wound sites demonstrated active healing with evidence of good microcirculation and progressing re-epithelialization.
Results: The patients required 6, 7, and 1 topical mVASC applications, respectively, at which point restored vascularity of the healing tissue was clinically evident, and PMVT treatment discontinued. In all three cases the wounds fully healed within several weeks after completing PMVT application. Patients have been followed one to four months after healing, and all wounds remain closed.
Discussion: Reversing the stalled wound pattern and changing the trajectory of healing towards wound resolution has been previously reported as a hallmark of PMVT treatment.3,4 Improvement of perfusion in these three refractory diabetic wounds are indicative of PMVT’s ability to support the repair and reconstruction of microvascular tissue, which in turn drove complete wound healing.

.png)