Case Series/Study
(CS-013) The Use of An Autologous Multilayered Leukocyte, Platelet and Fibrin Patch in Healing Diabetic Foot Ulcers in Patients who have Failed Other Advanced Modalities
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Warren Gude, MD – Medical Director, Wound and Hyperbarics, St. Luke's
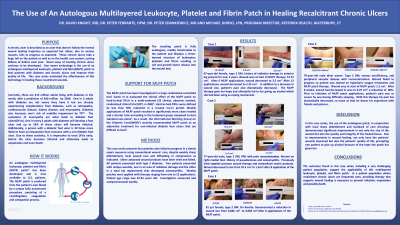
Introduction: Diabetic foot ulcers(DFUs) continue to be a huge dilemma in the United States with approximately 5% of patients with diabetes developing foot ulcers and 1% ending up with an amputation. Options for treating these wounds, preventing amputation and ultimately improving quality of life continue to be studied. The investigators of this study provide an analysis of eight patients treated with a novel autologous multilayered leukocyte, platelet, and fibrin patch (MLPF). The clinical team wanted to evaluate the impact of the MLPF patch on patients with Wagner grade 2-3 (DFUs) and low ABI’s. These patients have failed conventional treatment for DFUs, including cellular tissue products and offloading. Immune cells and growth factors are key components in acute wound healing but are often lacking in chronic wounds. The autologous multilayered leukocyte, platelet, and fibrin patch is an innovative treatment created by a unique process of centrifugation with just the patient’s blood. The patch is indicated for chronic wounds including DFUs.
Methods: The study presents eight patients who failed to progress in a timely repair sequence during conventional wound care despite weekly sharp debridement, local wound care, and offloading. In addition, some patients had proven critical limb ischemia. All patients presented with type 2 diabetes and peripheral arterial disease. Weekly patches were applied with therapy ranging from one to thirteen applications. Patient age range was 50-85 years old. Investigators measured and analyzed wounds weekly.
Results: Seven out of eight patients’ wounds closed with the use of the multilayered leukocyte, platelet, and fibrin patch with an average of eight weekly applications.
Discussion: In this eight-patient case series, the use of the autologous patch, in conjunction with local sharp debridement and offloading measures (total contact casting), demonstrated a better healing than previous treatments. Of the eight patients evaluated, seven healed with the patch during the twenty-week evaluation period. One patient underwent surgery after one application of the MLPF patch.
Methods: The study presents eight patients who failed to progress in a timely repair sequence during conventional wound care despite weekly sharp debridement, local wound care, and offloading. In addition, some patients had proven critical limb ischemia. All patients presented with type 2 diabetes and peripheral arterial disease. Weekly patches were applied with therapy ranging from one to thirteen applications. Patient age range was 50-85 years old. Investigators measured and analyzed wounds weekly.
Results: Seven out of eight patients’ wounds closed with the use of the multilayered leukocyte, platelet, and fibrin patch with an average of eight weekly applications.
Discussion: In this eight-patient case series, the use of the autologous patch, in conjunction with local sharp debridement and offloading measures (total contact casting), demonstrated a better healing than previous treatments. Of the eight patients evaluated, seven healed with the patch during the twenty-week evaluation period. One patient underwent surgery after one application of the MLPF patch.

.png)