Case Series/Study
(CS-015) Managing Skin Breakdown in Extremely Low Birthweight Babies Using a Unique Transforming Powder Technology
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Tammy Lichtman, RN, BSN, CWON – Assistant Nurse Manager, AdventHealth for Children
Introduction: Over 20 million newborns are low birth weight.1 Micro-preemies, or extremely low birthweight infants, are born at less than 26 weeks and are one of the most vulnerable patient populations. Their stratum corneum is only two cells thick and does not fully develop until late in the third trimester. The skin is especially fragile and easily traumatized by gentle adhesives, life support, monitoring equipment, and other necessary invasive procedures. “Touch-time” increases stress and exposure to infection through damaged or immature skin in an already immune-compromised host. Other skin related complications include energy demands from electrolyte imbalances, increased evaporative heat loss and the toxicity risk from external substances. Significant morbidity and mortality can be attributed to practices that cause either trauma to skin or alterations in normal skin function.2
Approaches to skin care in pre-term neonates varies considerably with location and clinical experiences. There is no single established guideline for neonatal skin care. Topical emollients, petrolatum ointments, humidification, plastic wraps, and transparent adhesive dressings have been used to treat weak or damaged skin barriers.
Methods: This case series presents 3 micro-preemies born at 22 weeks’ gestation (lowest birth weight of 1.5 pounds), who had large areas of denuded skin from tape trauma and were not responding to basic humidification. A novel extended wear transforming powder dressing (TPD), comprising of polymers similar to those used in contact lenses, was sprinkled over the damaged skin areas, transformed with warmed sterile saline, and covered with non-adhesive cover dressings. A total of two TPD applications were utilized and re-assessed over a 5 day period. TPD was left in place, but the cover dressings were changed as needed.
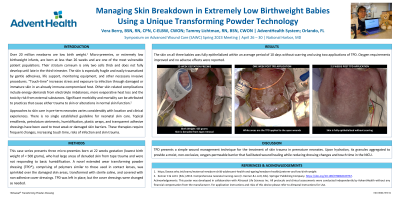
Results: The skin on all three babies was fully epithelialized within an average period of 10 days without scarring and using a single application of TPD. Oxygen requirements improved and no adverse effects were reported.
Discussion: TPD presents a simple wound management technique for the treatment of skin trauma in premature neonates. Upon hydration, its granules aggregate to provide a moist, non-occlusive, oxygen-permeable barrier that facilitated wound healing while reducing dressing changes and touch time in the NICU.
Approaches to skin care in pre-term neonates varies considerably with location and clinical experiences. There is no single established guideline for neonatal skin care. Topical emollients, petrolatum ointments, humidification, plastic wraps, and transparent adhesive dressings have been used to treat weak or damaged skin barriers.
Methods: This case series presents 3 micro-preemies born at 22 weeks’ gestation (lowest birth weight of 1.5 pounds), who had large areas of denuded skin from tape trauma and were not responding to basic humidification. A novel extended wear transforming powder dressing (TPD), comprising of polymers similar to those used in contact lenses, was sprinkled over the damaged skin areas, transformed with warmed sterile saline, and covered with non-adhesive cover dressings. A total of two TPD applications were utilized and re-assessed over a 5 day period. TPD was left in place, but the cover dressings were changed as needed.
Results: The skin on all three babies was fully epithelialized within an average period of 10 days without scarring and using a single application of TPD. Oxygen requirements improved and no adverse effects were reported.
Discussion: TPD presents a simple wound management technique for the treatment of skin trauma in premature neonates. Upon hydration, its granules aggregate to provide a moist, non-occlusive, oxygen-permeable barrier that facilitated wound healing while reducing dressing changes and touch time in the NICU.

.png)
