Case Series/Study
(CS-040) The Use of An Autologous Multilayered Leukocyte, Platelet and Fibrin Patch in Healing Recalcitrant Chronic Ulcers
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Peter Zdankiewicz, MD – Wound Center – Waterbury Health; Peter Ferrante, DPM – Co-Medical Director, Wound Center, Waterbury Health; David Knight, MD – Co-Medical Director, Wound Center, Waterbury Health
Introduction: A chronic ulcer is described as an ulcer that doesn’t follow the normal wound healing trajectory as expected but rather, due to various reasons, fails to progress as expected. These chronic ulcers takes a huge toll on the patient as well as on the health care system, costing billions of dollars each year. Novel ways of treating chronic ulcers continue to be developed. One newer technology is the use of an autologous multilayered leukocyte, platelet and fibrin patch to heal patients with diabetes and chronic ulcers and improve their quality of life. This case series evaluated the effectiveness of this technology in healing these recalcitrant wounds.
Methods: The study presents five patients who failed to progress in a timely repair sequence during conventional wound care despite weekly sharp debridement, local wound care, and offloading or compression as indicated. Other advanced wound products had been tried and failed. All patients presented with type 2 diabetes. Two patients presented with unique wounds, one in an area of radiation damage and the other in a total hip replacement that developed osteomyelitis. Weekly patches were applied with therapy ranging from one to thirteen applications. Patient age range was 67-81 years old. Investigators measured and analyzed wounds weekly.
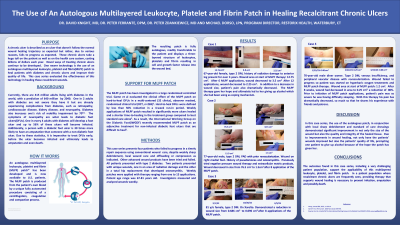
Results: The patient with the area of radiation damage showed significant improvement after failing to improve for the last three years, decreasing 92% in size after 12 applications of the autologous multilayered leukocyte, platelet, and fibrin patch. The patient who presented with the hip replacement wound decreased 40% in approximately 5 weeks with the use of the patch but then unfortunately was lost to follow-up. A third patient with a diabetic foot ulcer decreased in size from 26 cm3 to 0.13 cm3 after 8 applications of the patch. Another patient, also with a diabetic foot ulcer, demonstrated a reduction in wound size from 0.686 cm3 to 0.096 cm3 with 8 applications of the patch.
Discussion: In this case series, the use of the autologous patch, in conjunction with local sharp debridement and standard of care dressings included offloading as appropriate, demonstrated significant improvement in not only the size of the wound but also the quality and integrity of the healed tissue. Due to improvements in wound healing, not only have the patients’ wounds improved but the patients’ quality of life, prompting one patient to give up alcohol because of the hope the patch has given her.
Methods: The study presents five patients who failed to progress in a timely repair sequence during conventional wound care despite weekly sharp debridement, local wound care, and offloading or compression as indicated. Other advanced wound products had been tried and failed. All patients presented with type 2 diabetes. Two patients presented with unique wounds, one in an area of radiation damage and the other in a total hip replacement that developed osteomyelitis. Weekly patches were applied with therapy ranging from one to thirteen applications. Patient age range was 67-81 years old. Investigators measured and analyzed wounds weekly.
Results: The patient with the area of radiation damage showed significant improvement after failing to improve for the last three years, decreasing 92% in size after 12 applications of the autologous multilayered leukocyte, platelet, and fibrin patch. The patient who presented with the hip replacement wound decreased 40% in approximately 5 weeks with the use of the patch but then unfortunately was lost to follow-up. A third patient with a diabetic foot ulcer decreased in size from 26 cm3 to 0.13 cm3 after 8 applications of the patch. Another patient, also with a diabetic foot ulcer, demonstrated a reduction in wound size from 0.686 cm3 to 0.096 cm3 with 8 applications of the patch.
Discussion: In this case series, the use of the autologous patch, in conjunction with local sharp debridement and standard of care dressings included offloading as appropriate, demonstrated significant improvement in not only the size of the wound but also the quality and integrity of the healed tissue. Due to improvements in wound healing, not only have the patients’ wounds improved but the patients’ quality of life, prompting one patient to give up alcohol because of the hope the patch has given her.

.png)