Case Series/Study
(DLS-018) Application of Umbilical Cord Tissue Allografts in Reduction Mammoplasty Wound: A Case Study
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Naomi Lambert, BS – Technical Writer, Regenative Labs
Introduction: Nearly 15 million patients undergo cosmetic surgery in the United States each year, with breast augmentations such as implants, lifts, or reductions being some of the most common procedures. The most common complications of these procedures are scarring and infection at the incision site, which often necessitates expensive corrective surgery. After significant weight loss, the patient in this study underwent an elective lower body lift in conjunction with a breast reduction and nipple-areolar transplant. The patient experienced postoperative wound dehiscence, creating a large open wound, warranting rapid wound closure to avoid further pain and infection. The patient was treated for eight weeks with conservative measures. After eight weeks of failed attempts to close her wound, she was referred for specialist care.
Methods: Upon initial examination, the donor site wound measured 3.5 cm x 3.5 cm x 1.25 cm deep with no sign of epithelialization. The patient received a single dose of Wharton’s jelly flowable perinatal tissue allograft and twelve hyperbaric oxygen therapy treatments over seven weeks
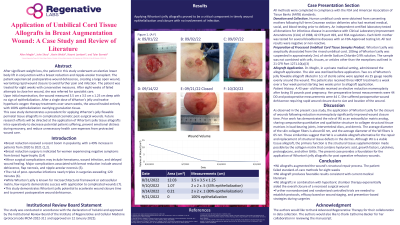
Results: Upon application on September 2, 2022, the wound measured 3.50 cm x 3.50 cm and 1.25 cm deep. Upon the first follow-up on September 10, 2022, the wound measured 2.0 cm x 2.0 cm and 0.5 cm deep with 43% epithelialization. At the second follow-up visit, the wound was entirely closed with some discoloration. At the final visit on October 20, 2022, the wound area had returned to normal coloration with no scarring.
Discussion: This case study demonstrates a precedent for the application of Wharton’s jelly flowable allografts in complicated cosmetic post-surgical wounds. This case provides evidence that WJ could be a suitable allograft alternative for the repair of structural tissue defects in the dermis. Future efforts will be directed at applying Wharton’s jelly allografts on a preventative basis. Preventative applications could be in stage 2 pressure sores, in the region of recurrent chronic venous insufficiency ulcers between stages of tenuous healing, prior to joint replacement in patients with immune-compromised states, or prior to surgical intervention in patients with a known history of postoperative infections. The obvious goal is to prevent needless patient suffering and reduce unnecessary healthcare costs.
Methods: Upon initial examination, the donor site wound measured 3.5 cm x 3.5 cm x 1.25 cm deep with no sign of epithelialization. The patient received a single dose of Wharton’s jelly flowable perinatal tissue allograft and twelve hyperbaric oxygen therapy treatments over seven weeks
Results: Upon application on September 2, 2022, the wound measured 3.50 cm x 3.50 cm and 1.25 cm deep. Upon the first follow-up on September 10, 2022, the wound measured 2.0 cm x 2.0 cm and 0.5 cm deep with 43% epithelialization. At the second follow-up visit, the wound was entirely closed with some discoloration. At the final visit on October 20, 2022, the wound area had returned to normal coloration with no scarring.
Discussion: This case study demonstrates a precedent for the application of Wharton’s jelly flowable allografts in complicated cosmetic post-surgical wounds. This case provides evidence that WJ could be a suitable allograft alternative for the repair of structural tissue defects in the dermis. Future efforts will be directed at applying Wharton’s jelly allografts on a preventative basis. Preventative applications could be in stage 2 pressure sores, in the region of recurrent chronic venous insufficiency ulcers between stages of tenuous healing, prior to joint replacement in patients with immune-compromised states, or prior to surgical intervention in patients with a known history of postoperative infections. The obvious goal is to prevent needless patient suffering and reduce unnecessary healthcare costs.

.png)
