Case Series/Study
(DLS-025) Conversion of a Fasciocutaneous Reverse Sural Artery Flap to an Adipofascial Flap for Flap Salvage in the Treatment of Chronic Calcaneal Osteomyelitis: A Case Study
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Brent Bernstein, DPM, FACFAS, FAPWCA – Limb Preservation Fellowship Director, Podiatry, St. Luke's University Health Network; Ruben nunez, DPM – Foot and Ankle Surgeon, Foot and Ankle Specialists of New Mexico
Introduction: The application of the reverse sural artery flap in soft tissue reconstruction of the heel is becoming increasingly more commonplace in the podiatric surgery realm. Known to be useful for covering defects of the lower third of the leg, ankle and hindfoot, this case specifically looks at its implication in the coverage of a chronic Wagner grade 4 heel ulcer in a patient with chronic calcaneal osteomyelitis. We report on the clinical result of proceeding with flap coverage in a patient with a less than optimal health condition as an alternative to more proximal amputation.
Methods: The patient is a 52 year male with insulin-dependent type 2 Diabetes, hypertension and peripheral vascular disease due to an extensive history of smoking. First, a left lower extremity angioplasty of the anterior tibial and posterior tibial arteries was performed in order to optimize two vessel run off into the left foot for optimal healing. Due to having only two vessels feeding the lower limb, the decision was made to delay insetting of the flap for one week to allow for choke vessels to dilate and for prevention of venous congestion. The delayed flap procedure was performed which involved harvesting a fasciocutaneous block of tissue fed by consistent distal perforators of the peroneal artery and laying it on the donor site atop of bilayered dermal tissue to prevent re-adherence. Due to venous congestion during the delay period, the decision was made to fully de-epithelialize the paddle into an adipofascial flap with application of dermal matrix bilayer and subsequent skin grafting.
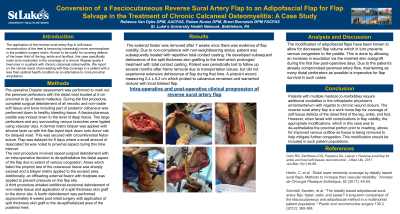
Results: Approximately 6 months after insetting, the converted adipofascial flap as well as the split thickness skin graft took well and without complication. However, the distal tip showed pinpoint necrosis down to deep fascia which subsequently warranted local wound care, including total contact casting, and ultimately local bilobed flap coverage.
Discussion: Wound healing in patients with challenging co-morbidities requires collaboration and a multi-disciplinary approach for the best chance at limb salvage. Additionally, salvaging a failing flap with additional measures such as de-epithelialization should be a choice plan for the orthoplastic surgeon who is presented with such a complication.
Methods: The patient is a 52 year male with insulin-dependent type 2 Diabetes, hypertension and peripheral vascular disease due to an extensive history of smoking. First, a left lower extremity angioplasty of the anterior tibial and posterior tibial arteries was performed in order to optimize two vessel run off into the left foot for optimal healing. Due to having only two vessels feeding the lower limb, the decision was made to delay insetting of the flap for one week to allow for choke vessels to dilate and for prevention of venous congestion. The delayed flap procedure was performed which involved harvesting a fasciocutaneous block of tissue fed by consistent distal perforators of the peroneal artery and laying it on the donor site atop of bilayered dermal tissue to prevent re-adherence. Due to venous congestion during the delay period, the decision was made to fully de-epithelialize the paddle into an adipofascial flap with application of dermal matrix bilayer and subsequent skin grafting.
Results: Approximately 6 months after insetting, the converted adipofascial flap as well as the split thickness skin graft took well and without complication. However, the distal tip showed pinpoint necrosis down to deep fascia which subsequently warranted local wound care, including total contact casting, and ultimately local bilobed flap coverage.
Discussion: Wound healing in patients with challenging co-morbidities requires collaboration and a multi-disciplinary approach for the best chance at limb salvage. Additionally, salvaging a failing flap with additional measures such as de-epithelialization should be a choice plan for the orthoplastic surgeon who is presented with such a complication.

.png)
