Case Series/Study
(CS-131) Dehydrated Human Umbilical Cord Allografts For The Treatment Of A Dog Bite Wound With Significant Tissue Loss: A Clinical Perspective
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Cierra Rangel, FNP – St. Mark's Hospital – HCA Healthcare; Wendy Skousen, RN – St. Mark's Hospital – HCA Healthcare
Introduction: In the United States more than 4.5 million people are bitten by dogs annually, and more than 800,000 receive medical attention for dog bites, according to the U.S. Centers for Disease Control (CDC). In 2020, a report released by the American Society of Plastic Surgeons, revealed that there were over 47,000 reconstructive procedures related to dog bites. The goal of this case report is to highlight the use of Dehydrated Human Umbilical Cord (DHUC) in the treatment of an unprovoked dog bite resulting in significant tissue loss to the left wrist.
Methods:
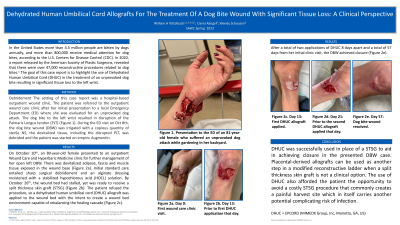
The setting of this case report was a hospital-based outpatient wound clinic. The patient was referred to the outpatient wound care clinic after her initial presentation to a local Emergency Department where she was evaluated for an unprovoked dog attack. The dog bite to the left wrist resulted in disruption of the Palmaris Longus tendon (PLT) (Figure 1). During the ED visit on Oct 8th, the dog bite wound (DBW) was irrigated with a copious amount of sterile NS, the devitalized tissue, including the disrupted PLT, was debrided and the patient was started on empiric Augmentin.
Results:
On October 10th an 80-year-old female was presented to an outpatient Wound care and Hyperbaric Medicine clinic for further management of her open left DBW. There was devitalized adipose, fascia and muscle tissue exposed in the wound base (Figure 2a). Initial standard care entailed surgical debridement and an alginate dressing moistened with HOCL. By October 26th the wound bed was prepared to receive a split thickness skin graft (STSG) (Figure 2b). However, the patient refused, so a dehydrated human umbilical cord (DHUC) allograft was applied to the wound bed with the intent to create a wound bed environment capable of rebalancing the healing cascade (Figure 2c). After a total of two applications of DHUC 8 days apart and a total of 57 days from her initial visit the DBW achieved closure (Figure 2e).
Discussion:
DHUC was successfully used in place of a STSG to aid in achieving closure in the presented DBW case. Placental-derived allografts, such as DHUC, can be used as another step in a modified reconstructive ladder when a STSG is not a clinical option. The use of DHUC also afforded the patient the opportunity to avoid a costly STSG procedure that creates a painful harvest site which itself carries another potential complicating risk of infection.
Methods:
The setting of this case report was a hospital-based outpatient wound clinic. The patient was referred to the outpatient wound care clinic after her initial presentation to a local Emergency Department where she was evaluated for an unprovoked dog attack. The dog bite to the left wrist resulted in disruption of the Palmaris Longus tendon (PLT) (Figure 1). During the ED visit on Oct 8th, the dog bite wound (DBW) was irrigated with a copious amount of sterile NS, the devitalized tissue, including the disrupted PLT, was debrided and the patient was started on empiric Augmentin.
Results:
On October 10th an 80-year-old female was presented to an outpatient Wound care and Hyperbaric Medicine clinic for further management of her open left DBW. There was devitalized adipose, fascia and muscle tissue exposed in the wound base (Figure 2a). Initial standard care entailed surgical debridement and an alginate dressing moistened with HOCL. By October 26th the wound bed was prepared to receive a split thickness skin graft (STSG) (Figure 2b). However, the patient refused, so a dehydrated human umbilical cord (DHUC) allograft was applied to the wound bed with the intent to create a wound bed environment capable of rebalancing the healing cascade (Figure 2c). After a total of two applications of DHUC 8 days apart and a total of 57 days from her initial visit the DBW achieved closure (Figure 2e).
Discussion:
DHUC was successfully used in place of a STSG to aid in achieving closure in the presented DBW case. Placental-derived allografts, such as DHUC, can be used as another step in a modified reconstructive ladder when a STSG is not a clinical option. The use of DHUC also afforded the patient the opportunity to avoid a costly STSG procedure that creates a painful harvest site which itself carries another potential complicating risk of infection.

.png)