Case Series/Study
(CS-123) Clinical Application of a Synthetic Hybrid-Scale Fiber Matrix* in a Dehisced Ankle Wound with Exposed Tendon
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Introduction: Ankle fractures are a common injury and often require surgical repair.1 The main postoperative complication seen with these repairs are surgical site dehiscence and infection.1 When these complications result in an open wound with exposed structures such as tendons, they become increasingly difficult to manage due to the avascular nature of these structures.2 In this present case study, a biodegradable synthetic hybrid-scale fiber matrix, with a size and structure similar to native human extracellular matrix,3 was utilized to achieve total wound closure in a dehisced ankle wound with exposed tendon by encouraging neovascularization and cellular infiltration.
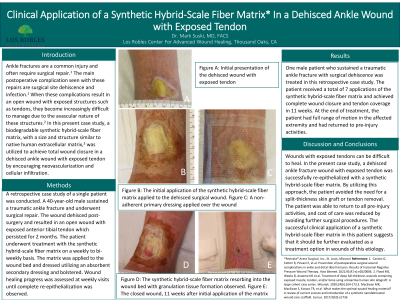
Methods: A retrospective case study of a single patient was conducted. A 40-year-old male sustained a traumatic ankle fracture and underwent surgical repair. The wound dehisced post-surgery and resulted in an open wound with exposed anterior tibial tendon which persisted for 2 months. The patient underwent treatment with the synthetic hybrid-scale fiber matrix on a weekly to bi-weekly basis. The matrix was applied to the wound bed and dressed utilizing an absorbent secondary dressing and bolstered. Wound healing progress was assessed at weekly visits until complete re-epithelialization was observed
Results: One male patient who sustained a traumatic ankle fracture with surgical dehiscence was treated in this retrospective case study. The patient received a total of 7 applications of the synthetic hybrid-scale fiber matrix and achieved complete wound closure and tendon coverage in 11 weeks. At the end of treatment, the patient had full range of motion in the affected extremity and had returned to pre-injury activities.
Discussion: Wounds with exposed tendons can be difficult to heal. In the present case study, a dehisced ankle fracture wound with exposed tendon was successfully re-epithelialized with a synthetic hybrid-scale fiber matrix. By utilizing this approach, the patient avoided the need for a split-thickness skin graft or tendon removal. The patient was able to return to all pre-injury activities, and cost of care was reduced by avoiding further surgical procedures. The successful clinical application of a synthetic hybrid-scale fiber matrix in this patient suggests that it should be further evaluated as a treatment option in wounds of this etiology.
Methods: A retrospective case study of a single patient was conducted. A 40-year-old male sustained a traumatic ankle fracture and underwent surgical repair. The wound dehisced post-surgery and resulted in an open wound with exposed anterior tibial tendon which persisted for 2 months. The patient underwent treatment with the synthetic hybrid-scale fiber matrix on a weekly to bi-weekly basis. The matrix was applied to the wound bed and dressed utilizing an absorbent secondary dressing and bolstered. Wound healing progress was assessed at weekly visits until complete re-epithelialization was observed
Results: One male patient who sustained a traumatic ankle fracture with surgical dehiscence was treated in this retrospective case study. The patient received a total of 7 applications of the synthetic hybrid-scale fiber matrix and achieved complete wound closure and tendon coverage in 11 weeks. At the end of treatment, the patient had full range of motion in the affected extremity and had returned to pre-injury activities.
Discussion: Wounds with exposed tendons can be difficult to heal. In the present case study, a dehisced ankle fracture wound with exposed tendon was successfully re-epithelialized with a synthetic hybrid-scale fiber matrix. By utilizing this approach, the patient avoided the need for a split-thickness skin graft or tendon removal. The patient was able to return to all pre-injury activities, and cost of care was reduced by avoiding further surgical procedures. The successful clinical application of a synthetic hybrid-scale fiber matrix in this patient suggests that it should be further evaluated as a treatment option in wounds of this etiology.

.png)