Case Series/Study
(CS-016) The application of marine Omega3 acellular dermal matrix wound for the management of Critical limb ischemia - the Asian experience
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Wuquan Deng, MD, PhD – Associate Professor of Endocrinology and Director, Endocrinology, Chongqing Emergency Medical Center; Alexis Lai, Bsc – Podiatrist, Podiatry, National university Hospital
Introduction: There are myriad of cellular and tissue-based products (CTPs) which have been recommended for the management of chronic diabetic wounds. Being rich in natural occuring omega 3 polysaturated fatty acid, the novel marine acellular dermal matrix has positioned itself in its unique vantage point over mammalian-based products. One such benefits is enhancing the host's antimicrobial properties, one that is usually lacking or hampered.
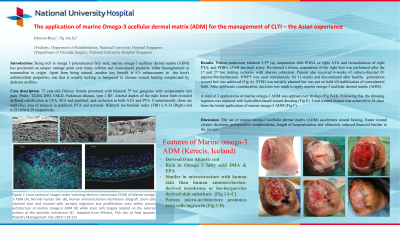
Methods: A case report of 72 years old Chinese female with bilateral critical limb ischemia and worsening rest pain in bilateral lower limb. Her past medical history includes, T2DM, ischemic heart disease, ESKD, Parkinson disease, type 2 respiratory failure. Arterial duplex of the right lower limb revealed diffused calcification in common femoral (CF), profunda, superficial femoral (SF) and popliteal, and occlusion in anterior tibial (AT) and posterior tibial (PT). Contralaterally, there are multi-foci area of stenosis in popliteal, posterior tibial and peroneal artery. Toe-brachial index of the right and left side is 0.34 and 0.29 respectively.
Results: Patient underwent third to fifth amputation and POBA of proximal AT and retrograde recanalization of occluded PT of right lower limb. Subsequently, a revisional Lisfranc amputation of the right foot was performed after the 1st and 2nd toe turning ischemic with abscess collection. Meanwhile, she also underwent 3-5th ray amputation and POBA of peroneal artery of the left lower limb. She was also treated with 6-weeks of IV piperacillin/tazobactam which is sensitive against mixed growth of Escherichia coli and Bacteroides fragilis cultured from tissue specimen. Negative pressure wound therapy was utilised for 11-weeks and discontinued after a clean and granulation wound bed was achieved. Thereafter, split skin graft was planned but was put on hold till stabilization of left lower limb. After deliberate consideration, decision was made to apply Marine Omega3 acellular dermal matrix, of which the patient received a total of 2 applications over 10 days. Following this, the dressing regimen was replaced with hydrofiber-based wound dressing and total wound closure was achieved in 3-weeks.
Discussion: The use of marine acellular dermal matrix accelerates wound healing. Faster wound closure decreases perioperative complications, length of hospitalization and ultimately reduce financial burden to the patients.
Methods: A case report of 72 years old Chinese female with bilateral critical limb ischemia and worsening rest pain in bilateral lower limb. Her past medical history includes, T2DM, ischemic heart disease, ESKD, Parkinson disease, type 2 respiratory failure. Arterial duplex of the right lower limb revealed diffused calcification in common femoral (CF), profunda, superficial femoral (SF) and popliteal, and occlusion in anterior tibial (AT) and posterior tibial (PT). Contralaterally, there are multi-foci area of stenosis in popliteal, posterior tibial and peroneal artery. Toe-brachial index of the right and left side is 0.34 and 0.29 respectively.
Results: Patient underwent third to fifth amputation and POBA of proximal AT and retrograde recanalization of occluded PT of right lower limb. Subsequently, a revisional Lisfranc amputation of the right foot was performed after the 1st and 2nd toe turning ischemic with abscess collection. Meanwhile, she also underwent 3-5th ray amputation and POBA of peroneal artery of the left lower limb. She was also treated with 6-weeks of IV piperacillin/tazobactam which is sensitive against mixed growth of Escherichia coli and Bacteroides fragilis cultured from tissue specimen. Negative pressure wound therapy was utilised for 11-weeks and discontinued after a clean and granulation wound bed was achieved. Thereafter, split skin graft was planned but was put on hold till stabilization of left lower limb. After deliberate consideration, decision was made to apply Marine Omega3 acellular dermal matrix, of which the patient received a total of 2 applications over 10 days. Following this, the dressing regimen was replaced with hydrofiber-based wound dressing and total wound closure was achieved in 3-weeks.
Discussion: The use of marine acellular dermal matrix accelerates wound healing. Faster wound closure decreases perioperative complications, length of hospitalization and ultimately reduce financial burden to the patients.

.png)