Case Series/Study
(CS-036) Optimizing Skin Graft Success in Venous Leg Ulcers Using Aseptically Processed Dehydrated Allograft Placental Membrane
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Krista Bauer, RN, WCC, OMS,; Kari Day, RN, BSN, WCC; Ashley Wardman, CPPM, Surgical LPN-C
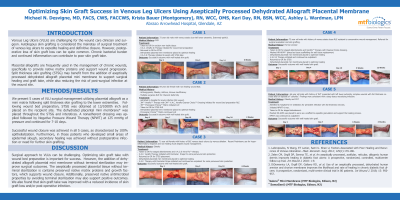
Introduction: Venous Leg Ulcers (VLUs) are challenging for the wound care clinician and surgeon. Autologous skin grafting is considered the mainstay of surgical treatment of venous leg ulcers to expedite healing and definitive closure. However, postoperative loss of skin graft loss can be quite common. Chronic bacterial burden and continued inflammation can contribute to poor skin graft take.
Methods: We present 5 cases of VLU surgical management utilizing placental allograft as a mini matrix following split thickness skin grafting to the lower extremities. Following wound bed preparation, STSG was obtained at 13/1000th inch and placed on the recipient site. The dehydrated placental mini membrane was placed throughout the STSG and interstices. A nonadherent dressing was applied followed by Negative Pressure Wound Therapy (NPWT) at 125 mmHg of pressure and continued for 7-10 days.
Results: Successful healing was achieved in all 5 cases, as characterized by 100% epithelialization. Furthermore, in those patients who developed small areas of epidermal slough, secondary healing was achieved without postoperative infection or need for further skin grafting.
Discussion: Surgical approach to VLUs can be challenging. Optimizing skin graft success with wound bed preparation is important to success. However, the addition of dehydrated allograft placental mini membrane without terminal sterilization may improve surgical outcomes. While the exact mechanisms are not known, the aseptically processed placental tissue without terminal sterilization is known to maintain the inherent growth factors and native matrix proteins, which supports wound closure. Additionally, maintaining the antimicrobial effect by avoiding terminal sterilization may be another mechanism that contributes. We found that skin graft outcomes were improved with a reduced incidence of skin graft loss and or post operative infection.
Methods: We present 5 cases of VLU surgical management utilizing placental allograft as a mini matrix following split thickness skin grafting to the lower extremities. Following wound bed preparation, STSG was obtained at 13/1000th inch and placed on the recipient site. The dehydrated placental mini membrane was placed throughout the STSG and interstices. A nonadherent dressing was applied followed by Negative Pressure Wound Therapy (NPWT) at 125 mmHg of pressure and continued for 7-10 days.
Results: Successful healing was achieved in all 5 cases, as characterized by 100% epithelialization. Furthermore, in those patients who developed small areas of epidermal slough, secondary healing was achieved without postoperative infection or need for further skin grafting.
Discussion: Surgical approach to VLUs can be challenging. Optimizing skin graft success with wound bed preparation is important to success. However, the addition of dehydrated allograft placental mini membrane without terminal sterilization may improve surgical outcomes. While the exact mechanisms are not known, the aseptically processed placental tissue without terminal sterilization is known to maintain the inherent growth factors and native matrix proteins, which supports wound closure. Additionally, maintaining the antimicrobial effect by avoiding terminal sterilization may be another mechanism that contributes. We found that skin graft outcomes were improved with a reduced incidence of skin graft loss and or post operative infection.

.png)