Case Series/Study
(CS-057) Clinical Application of a Synthetic Hybrid-Scale Fiber Matrix* in a Chronic Diabetic Foot Wound
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Jean Chen-Vitulli, DPM – Endocrine Associates of West Village
Introduction: Non-healing lower extremity wounds can be challenging to treat, and often experience poor healing rates.1 A synthetic hybrid-scale fiber matrix (SHSFM) could be a novel treatment option in the management of these difficult wounds. The SHSFM is engineered to mimic the structure of native human extracellular matrix in both size and structure, therefore encouraging cellular infiltration and proliferation.2 The SHSFM then resorbs via hydrolysis at a controlled rate that matches tissue ingrowth.1-2 Prior studies of the SHSFM in lower extremity wounds have demonstrated healing rates of 75%-85% over a period of 12 weeks.1,3
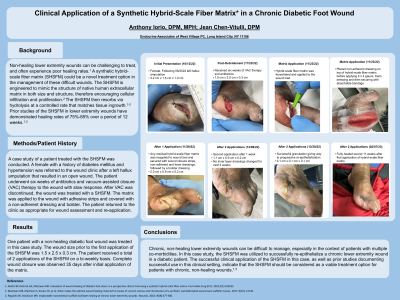
Methods: A case study of a patient treated with the SHSFM was conducted. A female with a history of diabetes mellitus and hypertension was referred to the wound clinic after a left hallux amputation that resulted in an open wound. The patient underwent six weeks of antibiotics and vacuum-assisted closure (VAC) therapy to the wound with slow response. After VAC was discontinued, the wound was treated with a SHSFM. The matrix was applied to the wound with adhesive strips and covered with a non-adherent dressing and bolster. The patient returned to the clinic as appropriate for wound assessment and re-application.
Results: One patient with a non-healing diabetic foot wound was treated in this case study. The wound size prior to the first application of the SHSFM was 1.5 x 2.5 x 0.3 cm. The patient received a total of 2 applications of the SHSFM on a bi-weekly basis. Complete wound closure was observed 35 days after initial application of the matrix.
Discussion: Chronic, non-healing lower extremity wounds can be difficult to manage, especially in the context of patients with multiple co-morbidities. In this case study, the SHSFM was utilized to successfully re-epithelialize a chronic lower extremity wound in a diabetic patient. The successful clinical application of the SHSFM in this case, as well as prior studies documenting successful use in this clinical setting, indicate that the SHSFM should be considered as a viable treatment option for patients with chronic, non-healing wounds.1,3
Methods: A case study of a patient treated with the SHSFM was conducted. A female with a history of diabetes mellitus and hypertension was referred to the wound clinic after a left hallux amputation that resulted in an open wound. The patient underwent six weeks of antibiotics and vacuum-assisted closure (VAC) therapy to the wound with slow response. After VAC was discontinued, the wound was treated with a SHSFM. The matrix was applied to the wound with adhesive strips and covered with a non-adherent dressing and bolster. The patient returned to the clinic as appropriate for wound assessment and re-application.
Results: One patient with a non-healing diabetic foot wound was treated in this case study. The wound size prior to the first application of the SHSFM was 1.5 x 2.5 x 0.3 cm. The patient received a total of 2 applications of the SHSFM on a bi-weekly basis. Complete wound closure was observed 35 days after initial application of the matrix.
Discussion: Chronic, non-healing lower extremity wounds can be difficult to manage, especially in the context of patients with multiple co-morbidities. In this case study, the SHSFM was utilized to successfully re-epithelialize a chronic lower extremity wound in a diabetic patient. The successful clinical application of the SHSFM in this case, as well as prior studies documenting successful use in this clinical setting, indicate that the SHSFM should be considered as a viable treatment option for patients with chronic, non-healing wounds.1,3

.png)