Case Series/Study
(CS-062) Management of Post-Mohs Micrographic Surgery Wounds with a Hypothermically Stored Amniotic Membrane: A Case Series
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Laura Pfendler, DPT
Introduction: Skin cancer is the most common form of cancer in the United States with an estimated 1 in 5 individuals affected in their lifetime1-3. Basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) are the most common skin cancers and account for a combined 5.4 million cases diagnosed each year4. Mohs Micrographic Surgery (MMS) is regarded as the most effective treatment for the management of BCC and SCC5. However, MMS can leave large tissue defects that may require skin grafts, flaps, or are left to heal by secondary intention6,7. Autologous skin grafts are the gold standard treatment but are limited by donor skin availability and donor site wounds bring the potential for added pain and scarring6,8. Skin substitutes may offer a solution for post-MMS wounds by eliminating the need for donor site wounds and supporting wound healing. This case series presents an alternative approach to managing post-MMS wounds with hypothermically stored amniotic membrane (HSAM)(a).
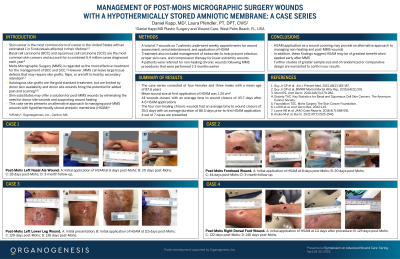
Methods: A case series of 7 post-MMS wounds on 7 patients with multiple comorbidities is presented. Four patients were referred for non-healing chronic wounds following MMS procedures that were performed 1-3 months earlier. All wounds underwent weekly appointments for wound assessment, serial debridement, and application of HSAM. Treatment also included management of bioburden to help prevent infection, proper skin care, and compression therapy for lower extremity wounds.
Results: The case series consisted of four females and three males with a mean age of 87.6 years. Mean wound size at first application of HSAM was 1.34 cm2. All wounds closed, with an average time to wound closure of 43.7 days. All patients received an average of 4.6 HSAM applications. The four non-healing chronic wounds had an average time to wound closure of 35.5 days with an average duration of 86.5 days prior to first HSAM application.
Discussion: HSAM application as a wound covering may provide an alternative approach to managing non-healing and post-MMS wounds. In addition, these findings suggest HSAM may be of greatest benefit when applied early after MMS. Further studies of greater sample size and of randomized or comparative design are warranted to confirm our results.
Methods: A case series of 7 post-MMS wounds on 7 patients with multiple comorbidities is presented. Four patients were referred for non-healing chronic wounds following MMS procedures that were performed 1-3 months earlier. All wounds underwent weekly appointments for wound assessment, serial debridement, and application of HSAM. Treatment also included management of bioburden to help prevent infection, proper skin care, and compression therapy for lower extremity wounds.
Results: The case series consisted of four females and three males with a mean age of 87.6 years. Mean wound size at first application of HSAM was 1.34 cm2. All wounds closed, with an average time to wound closure of 43.7 days. All patients received an average of 4.6 HSAM applications. The four non-healing chronic wounds had an average time to wound closure of 35.5 days with an average duration of 86.5 days prior to first HSAM application.
Discussion: HSAM application as a wound covering may provide an alternative approach to managing non-healing and post-MMS wounds. In addition, these findings suggest HSAM may be of greatest benefit when applied early after MMS. Further studies of greater sample size and of randomized or comparative design are warranted to confirm our results.

.png)