Case Series/Study
(CS-078) Pyoderma Gangrenosum: Dehydrated Human Amnion/Chorion Membrane, A Promising Approach To An Orphan Disease
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
William Tettelbach, MD, FACP, FIDSA, FUHM, MAPWCA – Executive Medical Director/Adjunct Assistant Professor, HCA Healthcare/Duke Univeraity School of Medicine; Allyn Forsyth, PhD – Director Medical Affairs Publications & Communications, MIMEDX Group, Inc
Introduction: Pyoderma gangrenosum (PG) is an often misdiagnosed painful inflammatory, ulcerative skin disorder. It is an orphan disease where standard wound treatments such as sharp surgical debridement are contraindicated. This retrospective case series sought to evaluate the application of dehydrated human amnion/chorion membrane (DHACM) as a skin substitute in cases that were refractory to a range of standard of care techniques including anti-inflammatory and immunosuppressive therapies.
Methods: The setting of this retrospective case series was a hospital-based outpatient dermatology clinic, the clinician was presented with three subjects with five refractory PG wounds referred by local wound care specialist. Subjects were provided standard treatments for PG, escalating from first line to third line anti-inflammatory and immunosuppressive topical and systemic agents. Informed consent was obtained from all participants. Subjects were transitioned to DHACM and wound sizes monitored till closure
Results: Patients were all female ages 45 to 76 years old, and each had previous diagnoses of at least one autoimmune disorder. Wounds were each located between the ankle to the knee, and sized from 12cm2 - 81cm2 at their largest. Wounds (n =5) for all three subjects had stalled during 2.5 months or more of standard therapies while waiting for insurance authorization for DHACM treatments. Subjects responded quickly to adjunctive DHACM applications with reductions in wound size and the cessation of pain medications. Wound closures were achieved for each patient.
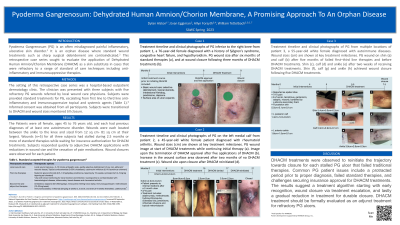
Example case: Treatment timeline and clinical photographs of PG inferior to the right knee from a 76-year-old female diagnosed with Sjögren’s syndrome, CHF, and hypothyroidism. PG reduced wound size after six months of standard therapies (Pic a), and at wound closure following three months of DHACM treatments (Pic b).
Discussion: DHACM treatments re-initiated the trajectory towards wound closure for each stalled PG ulcer that failed traditional therapies. Common patient issues include a protracted period prior to proper diagnosis, failed standard therapies, and challenges getting insurance approval for DHACM treatments. The results suggest a treatment algorithm starting with early recognition, wound closure via treatment escalation, and lastly a gradual reduction in treatment for durable closure. PG patients who were provided DHACM treatments in this case study, were able to halt pain medications and experienced closure of previously recalcitrant ulcers. DHACM treatment should be formally evaluated as an adjunct to PG ulcers that have remained refractory to more commonly used immunomodulating therapies.
Methods: The setting of this retrospective case series was a hospital-based outpatient dermatology clinic, the clinician was presented with three subjects with five refractory PG wounds referred by local wound care specialist. Subjects were provided standard treatments for PG, escalating from first line to third line anti-inflammatory and immunosuppressive topical and systemic agents. Informed consent was obtained from all participants. Subjects were transitioned to DHACM and wound sizes monitored till closure
Results: Patients were all female ages 45 to 76 years old, and each had previous diagnoses of at least one autoimmune disorder. Wounds were each located between the ankle to the knee, and sized from 12cm2 - 81cm2 at their largest. Wounds (n =5) for all three subjects had stalled during 2.5 months or more of standard therapies while waiting for insurance authorization for DHACM treatments. Subjects responded quickly to adjunctive DHACM applications with reductions in wound size and the cessation of pain medications. Wound closures were achieved for each patient.
Example case: Treatment timeline and clinical photographs of PG inferior to the right knee from a 76-year-old female diagnosed with Sjögren’s syndrome, CHF, and hypothyroidism. PG reduced wound size after six months of standard therapies (Pic a), and at wound closure following three months of DHACM treatments (Pic b).
Discussion: DHACM treatments re-initiated the trajectory towards wound closure for each stalled PG ulcer that failed traditional therapies. Common patient issues include a protracted period prior to proper diagnosis, failed standard therapies, and challenges getting insurance approval for DHACM treatments. The results suggest a treatment algorithm starting with early recognition, wound closure via treatment escalation, and lastly a gradual reduction in treatment for durable closure. PG patients who were provided DHACM treatments in this case study, were able to halt pain medications and experienced closure of previously recalcitrant ulcers. DHACM treatment should be formally evaluated as an adjunct to PG ulcers that have remained refractory to more commonly used immunomodulating therapies.

.png)