Case Series/Study
(CS-107) Cyclical Pressurized Topical Oxygen Therapy for the Treatment of Late Effect Radiation Wounds
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
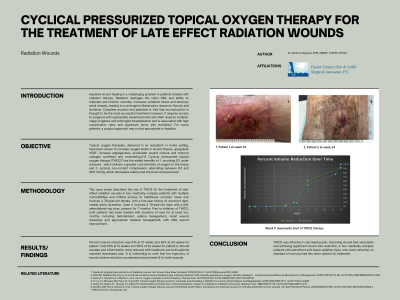
Introduction: Impaired wound healing is a challenging problem in patients treated with radiation therapy. Radiation damages the cell’s DNA and ability to replicate and function normally, increases oxidative stress and destroys small vessels, leading to a prolonged inflammatory response, fibrosis and ischemia. Complete excision and pedicled or free flap reconstruction is thought to be the most successful treatment; however, it requires access to surgeons with appropriate experience/skill and often requires multiple-stage surgeries and prolonged hospitalization and is associated with high complication rates and significant donor site morbidity.1 For some patients, a surgical approach may not be appropriate or feasible. Topical oxygen therapies, delivered in an outpatient or home setting, have been shown to increase oxygen levels in wound tissues, upregulate VEGF, increase angiogenesis, accelerate wound closure and improve collagen synthesis and remodeling.2–6 Cyclical pressurized topical oxygen therapy (CPTOT) has the added benefits of: 1. providing O2 under pressure, which delivers a greater concentration of oxygen to the tissue and 2. cyclical, non-contact compression, which decreases edema and improves local perfusion.
Methods: This case series describes the use of CPTOT for the treatment of late-effect radiation wounds in two medically complex patients with limited access to healthcare services. Case one involves a 76-year-old female, with a five-year history of recurrent right, medial ankle ulceration. Case 2 involves a 78-year-old male with a left, anterolateral leg ulcer, present for 7 months. Prior to initiation of CPTOT, both patients had been treated with standard of care for at least four weeks, including debridement, edema management, moist wound dressings and appropriate medical management, with little wound improvement.
Results: Percent volume reduction was 61% at 12 weeks and 92% at 24 weeks for patient 1 and 50% at 12 weeks and 79% at 24 weeks for patient 2. Wound exudate and inflammation were reduced with treatment and both patients reported decreased pain.
Discussion: CPTOT was effective in decreasing pain, improving wound bed vascularity and achieving significant wound size reduction, in two medically complex patients with late-effect soft tissue radiation injury, who were refractory to standard of care and had few other options for treatment.
Methods: This case series describes the use of CPTOT for the treatment of late-effect radiation wounds in two medically complex patients with limited access to healthcare services. Case one involves a 76-year-old female, with a five-year history of recurrent right, medial ankle ulceration. Case 2 involves a 78-year-old male with a left, anterolateral leg ulcer, present for 7 months. Prior to initiation of CPTOT, both patients had been treated with standard of care for at least four weeks, including debridement, edema management, moist wound dressings and appropriate medical management, with little wound improvement.
Results: Percent volume reduction was 61% at 12 weeks and 92% at 24 weeks for patient 1 and 50% at 12 weeks and 79% at 24 weeks for patient 2. Wound exudate and inflammation were reduced with treatment and both patients reported decreased pain.
Discussion: CPTOT was effective in decreasing pain, improving wound bed vascularity and achieving significant wound size reduction, in two medically complex patients with late-effect soft tissue radiation injury, who were refractory to standard of care and had few other options for treatment.

.png)