Case Series/Study
(DLS-021) Clinical Observations on the Use of a Novel Powder Dressing in the Treatment of Sickle Cell Associated Lower Extremity Wounds
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Amit Rao, M.D. – Project Manager, Surgery, Northwell Health; Christina del Pin, M.D. – Attending Physician, Surgery, Northwell Health; Marisa Ranire-Maguire, M.D. – Attending Physician, Surgery, Northwell Health; Kane Genser, M.D. – Fellow, Wound Care, Surgery, Northwell Health; Regina Matatova, M.S.N. – Nurse Practitioner, Wound Care, Surgery, Northwell Health; Julie Isgro, M.S.N. – Nurse Practitioner, Wound Care, Surgery, Northwell Health
Introduction: Sickle cell related wounds are notoriously difficult to heal. Challenges involved in treating these wounds typically involve managing pain, addressing vascular insufficiency and decreasing inflammation both peri-wound and in the wound. We describe the application of a novel powder dressing with unique properties to sickle cell anemia related wounds with positive results.
Methods: The clinical evidence of a novel power wound dressing has been demonstrated previously for wounds such as venous ulcers or diabetic foot ulcers. In this case study, the treatment regimen of two sickle cell ulcers is reviewed. The wounds were treated with a novel power wound dressing once weekly for four to eight weeks.
For each wound, the powder was applied according to manufacturers instructions where it transformed from a white powder into a translucent, flexible film on the wound bed. The dressing did not overlap onto tissue surrounding the wound.
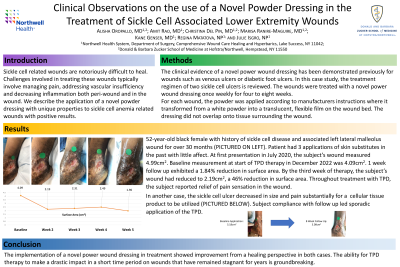
Results: 52-year-old black female with history of sickle cell disease and associated left lateral malleolus wound for over 30 months. Patient had 3 applications of skin substitutes in the past with little affect. At first presentation in July 2020, the subject’s wound measured 4.99cm2. Baseline measurement at start of TPD therapy in December 2022 was 4.09cm2. 1 week follow up exhibited a 1.84% reduction in surface area. By the third week of therapy, the subject’s wound had reduced to 2.19cm2, a 46% reduction in surface area. Throughout treatment with TPD, the subject reported relief of pain sensation in the wound.
In another case, the sickle cell ulcer decreased in size and pain substantially in order for a skin substitute to be utilized.
Discussion: The implementation of a novel power wound dressing in treatment showed improvement from a healing perspective in both cases. The ability for TPD therapy to make a drastic impact in a short time period on wounds that have remained stagnant for years is groundbreaking.
Methods: The clinical evidence of a novel power wound dressing has been demonstrated previously for wounds such as venous ulcers or diabetic foot ulcers. In this case study, the treatment regimen of two sickle cell ulcers is reviewed. The wounds were treated with a novel power wound dressing once weekly for four to eight weeks.
For each wound, the powder was applied according to manufacturers instructions where it transformed from a white powder into a translucent, flexible film on the wound bed. The dressing did not overlap onto tissue surrounding the wound.
Results: 52-year-old black female with history of sickle cell disease and associated left lateral malleolus wound for over 30 months. Patient had 3 applications of skin substitutes in the past with little affect. At first presentation in July 2020, the subject’s wound measured 4.99cm2. Baseline measurement at start of TPD therapy in December 2022 was 4.09cm2. 1 week follow up exhibited a 1.84% reduction in surface area. By the third week of therapy, the subject’s wound had reduced to 2.19cm2, a 46% reduction in surface area. Throughout treatment with TPD, the subject reported relief of pain sensation in the wound.
In another case, the sickle cell ulcer decreased in size and pain substantially in order for a skin substitute to be utilized.
Discussion: The implementation of a novel power wound dressing in treatment showed improvement from a healing perspective in both cases. The ability for TPD therapy to make a drastic impact in a short time period on wounds that have remained stagnant for years is groundbreaking.

.png)

