Case Series/Study
(DLS-022) Neurostimulation treatment in ‘End Stage Peripheral Vascular Disease’ with no revascularization option can achieve limb salvage and treat disabling claudication by improving blood flow into the affected limb: Review of cases
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Muntasha Quddus, BSc in Clinical Medicine; BMBS – FY1 (Foundation year 1), Trauma & Orthopaedics, Leeds Royal Infirmary; Tanjim Quddus, BSc in Surgery – 4th Year Medical Student, MBChB course, Hull York Medical University, UK; Asmita Singh, MBChB student – Final year Medical Student, MBChB course, Manchester Medical University, UK
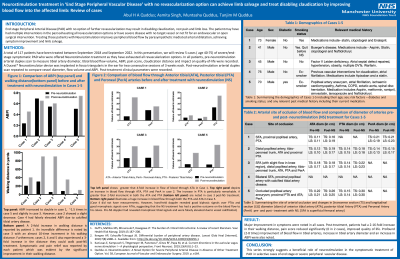
Introduction: End stage Peripheral Arterial Disease (PAD) with no option of further revascularization may result in disabling claudication, rest pain and limb loss. The patient may have had multiple interventions in the past exhausting all revascularization options or have severe disease with no target vessel or not fit for an endovascular or open surgical intervention. Treating those patients with Neurostimulation improves peripheral blood flow by parasympathetic mediated arterial dilatation, achieving symptom improvement and limb salvage.
Methods: A total of 117 patients have been treated between September 2018 and September 2022. In this presentation, we will review 6 cases (5 males, 1 female; age 40-75) of severe/end-stage symptomatic PAD who were offered Neurostimulation treatment as they have exhausted all revascularization options. In all patients, pre-neurostimulation arterial duplex scan to measure tibial artery diameter, tibial blood flow volume, ABPI, pain score, claudication distance and impact on quality-of-life were recorded. A Ducest* Neurostimulator device was implanted in fossa triangularis in the ear for two consecutive sessions of 3 weeks each. Post-neurostimulation arterial duplex scan repeated to compare vessel diameter, flow volume and ABPI. Post-treatment clinical parameters were recorded.
Results: Major Improvement in symptoms were noted in all cases. Post-treatment, patients had a 2-16-fold increase in their walking distance, pain score reduced significantly (0 in 2 cases), improved quality of life. Profound (2-8 times) improvement of blood flow in tibial arteries, increase in tibial artery diameter and an increase in ABPI were also noted.
Discussion: This case series strongly suggests a beneficial role of neurostimulation treatment in selective cases of extensive or end stage PAD.
Graphs showing improved Tibial artery Flow Volume, Increase in Tibial artery Diameter and Improved ABPI following Neurostimulation treatment will be presented.
Methods: A total of 117 patients have been treated between September 2018 and September 2022. In this presentation, we will review 6 cases (5 males, 1 female; age 40-75) of severe/end-stage symptomatic PAD who were offered Neurostimulation treatment as they have exhausted all revascularization options. In all patients, pre-neurostimulation arterial duplex scan to measure tibial artery diameter, tibial blood flow volume, ABPI, pain score, claudication distance and impact on quality-of-life were recorded. A Ducest* Neurostimulator device was implanted in fossa triangularis in the ear for two consecutive sessions of 3 weeks each. Post-neurostimulation arterial duplex scan repeated to compare vessel diameter, flow volume and ABPI. Post-treatment clinical parameters were recorded.
Results: Major Improvement in symptoms were noted in all cases. Post-treatment, patients had a 2-16-fold increase in their walking distance, pain score reduced significantly (0 in 2 cases), improved quality of life. Profound (2-8 times) improvement of blood flow in tibial arteries, increase in tibial artery diameter and an increase in ABPI were also noted.
Discussion: This case series strongly suggests a beneficial role of neurostimulation treatment in selective cases of extensive or end stage PAD.
Graphs showing improved Tibial artery Flow Volume, Increase in Tibial artery Diameter and Improved ABPI following Neurostimulation treatment will be presented.

.png)
