Case Series/Study
(DLS-023) Using a novel polylactic acid dermal matrix for achieving closure and limb salvage in hard-to-heal wounds
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Brock Liden, DPM; Christian Planck, CEO; Max Froehlich, MD; Darren Doerr, MBA
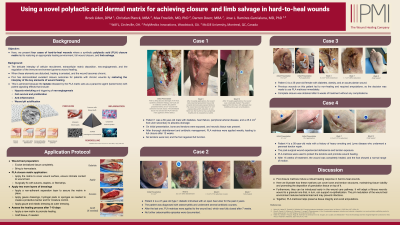
Introduction: The interplay of cellular recruitment, extracellular matrix deposition, neoangiogenesis, and the regulation of the immune environment governs wound healing. When these elements are disturbed, healing is arrested. Here, we present five cases of hard-to-heal wounds where a synthetic polylactic acid (PLA) closure matrix led to restoring an appropriate healing environment, full wound closure, and limb salvage.
Methods: Patients received weekly applications of PLA matrices that enhance cellular growth, promote neo-vascularization, and modulate the inflammatory and acid-base environments.
Results: Patient 1 had diabetes, heart failure, peripheral arterial disease, and a 25.2 cm2 foot ulcer secondary to abscess drainage. On initial presentation, bone and tendons were exposed, and necrotic tissue was present. PLA matrices were applied weekly, leading to full closure after 12 weeks. No tendons were lost, and the foot regained full function. Patient 2 is type 1 diabetic individual with an open heel ulcer for the past 2 years. The patient was diagnosed with osteomyelitis and underwent several antibiotic courses. After the last one, PLA matrices were applied to the wound bed, which was fully closed after 7 weeks. No further osteomyelitis episodes were documented. Patient 3 has diabetes, obesity, and an acute plantar wound. Previous wounds on this patient led to non-healing and required amputations, so we used PLA matrices immediately. Complete closure was obtained after 9 weeks without complications. Patient 4 is a heavy smoker with Lyme disease who underwent a peroneal tendon repair that dehiscenced and exposed the tendon. PLA matrices were used to protect the tendons and promote healing after 15 weeks. Finally, patient 5 was referred to our clinic because of a 35 cm2 post-surgical wound dehiscence following Achilles tendon repair that was refractive to treatment, appeared atrophic and with an exposed tendon. After 2 weeks of treatment, full tendon coverage with granulation tissue was achieved, and 3 weeks later, the wound was closed.
Discussion: PLA closure matrices induce a robust healing response in hard-to-heal wounds. Here we illustrate how these matrices can cover bone and tendon structures, maintaining tissue viability and promoting the deposition of granulation tissue on top of it. Furthermore, they can be introduced early in the wound care pathway. It will adapt a fibrous necrotic wound to a granular one that, in turn, can support re-epithelization. The pH modulation of the wound bed environment reduces bacterial load and may prevent infections. Together, it helps preserve tissue integrity and avoid amputations.
Methods: Patients received weekly applications of PLA matrices that enhance cellular growth, promote neo-vascularization, and modulate the inflammatory and acid-base environments.
Results: Patient 1 had diabetes, heart failure, peripheral arterial disease, and a 25.2 cm2 foot ulcer secondary to abscess drainage. On initial presentation, bone and tendons were exposed, and necrotic tissue was present. PLA matrices were applied weekly, leading to full closure after 12 weeks. No tendons were lost, and the foot regained full function. Patient 2 is type 1 diabetic individual with an open heel ulcer for the past 2 years. The patient was diagnosed with osteomyelitis and underwent several antibiotic courses. After the last one, PLA matrices were applied to the wound bed, which was fully closed after 7 weeks. No further osteomyelitis episodes were documented. Patient 3 has diabetes, obesity, and an acute plantar wound. Previous wounds on this patient led to non-healing and required amputations, so we used PLA matrices immediately. Complete closure was obtained after 9 weeks without complications. Patient 4 is a heavy smoker with Lyme disease who underwent a peroneal tendon repair that dehiscenced and exposed the tendon. PLA matrices were used to protect the tendons and promote healing after 15 weeks. Finally, patient 5 was referred to our clinic because of a 35 cm2 post-surgical wound dehiscence following Achilles tendon repair that was refractive to treatment, appeared atrophic and with an exposed tendon. After 2 weeks of treatment, full tendon coverage with granulation tissue was achieved, and 3 weeks later, the wound was closed.
Discussion: PLA closure matrices induce a robust healing response in hard-to-heal wounds. Here we illustrate how these matrices can cover bone and tendon structures, maintaining tissue viability and promoting the deposition of granulation tissue on top of it. Furthermore, they can be introduced early in the wound care pathway. It will adapt a fibrous necrotic wound to a granular one that, in turn, can support re-epithelization. The pH modulation of the wound bed environment reduces bacterial load and may prevent infections. Together, it helps preserve tissue integrity and avoid amputations.

.png)
