Case Series/Study
(CS-124) Successful Diabetic Limb Salvage Utilizing a Novel Fish Skin Graft
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Introduction: Total knee arthroplasty is associated with wound complications including dehiscence and surgical site infections (SSI)1. Metabolic disease and trauma augment post operative complica-tions1,2. To avoid amputations in high-risk patients’ health care providers have turned to advanced biologics. The purpose of this case study was to determine the effectiveness of novel fish skin graft (FSG) for the treatment of surgical dehiscence.
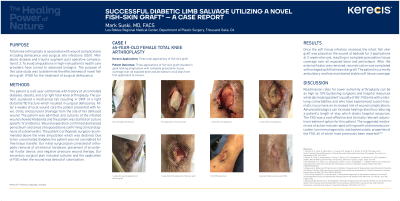
Methods: The patient is a 65-year-old female with history of uncontrolled diabetes, obesity, and h/o right total knee arthroplasty. The patient sustained a mechanical fall resulting in ORIF of a right distal tib/fib fracture. Her immediate postoperative course was complicated by dehiscence of her anteromedial incision, recalcitrant to 6 weeks of local wound care. One month after the initial fall, the patient was admitted with fever, chills, and purulent drainage from the site of her dehisced wound. At the time of admission, a new right proximal tibia fracture inferior to the tibial stem of her right knee prosthesis was seen on Xray. Upon questioning the patient stated that she had sustained an interval fall during rehab. Cultures of the infected wound grew Klebsiella and the patient was started on culture specific antibiotics. Further diagnostic imaging revealed malunion of her initial tibial fracture. Wound exploration confirmed exposed periosteum confirming clinical diagnosis of osteomyelitis. The patient's orthopedic surgeon recommended above the knee amputation. The patient was not considered not considered for free tissue transfer due to her uncontrolled diabetes, therefore our initial surgical plan consisted of orthopedic removal of all internal hardware, placement of an external fixator device, and negative pressure wound therapy.
Results: Once the soft tissue infection resolved, the intact fish skin graft was placed on the wound at bedside for 3 applications at 2-week intervals, resulting in complete granulation tissue coverage over all exposed bone and periosteum. After the external fixator was removed, reconstruction was completed with a staged split thickness skin graft.
Discussion: Readmission rates for lower extremity arthroplasty can be as high as 15% burdening surgeons and hospital resources while decreasing patient’s quality of life. The FSG was a cost-effective and clinically relevant adjunctive treatment option for this patient. The suggested mechanisms of action include rapid cell ingrowth and neovascularization, low immunogenicity, and bacteriostatic properties of the FSG, all of which have previously been reported.
Methods: The patient is a 65-year-old female with history of uncontrolled diabetes, obesity, and h/o right total knee arthroplasty. The patient sustained a mechanical fall resulting in ORIF of a right distal tib/fib fracture. Her immediate postoperative course was complicated by dehiscence of her anteromedial incision, recalcitrant to 6 weeks of local wound care. One month after the initial fall, the patient was admitted with fever, chills, and purulent drainage from the site of her dehisced wound. At the time of admission, a new right proximal tibia fracture inferior to the tibial stem of her right knee prosthesis was seen on Xray. Upon questioning the patient stated that she had sustained an interval fall during rehab. Cultures of the infected wound grew Klebsiella and the patient was started on culture specific antibiotics. Further diagnostic imaging revealed malunion of her initial tibial fracture. Wound exploration confirmed exposed periosteum confirming clinical diagnosis of osteomyelitis. The patient's orthopedic surgeon recommended above the knee amputation. The patient was not considered not considered for free tissue transfer due to her uncontrolled diabetes, therefore our initial surgical plan consisted of orthopedic removal of all internal hardware, placement of an external fixator device, and negative pressure wound therapy.
Results: Once the soft tissue infection resolved, the intact fish skin graft was placed on the wound at bedside for 3 applications at 2-week intervals, resulting in complete granulation tissue coverage over all exposed bone and periosteum. After the external fixator was removed, reconstruction was completed with a staged split thickness skin graft.
Discussion: Readmission rates for lower extremity arthroplasty can be as high as 15% burdening surgeons and hospital resources while decreasing patient’s quality of life. The FSG was a cost-effective and clinically relevant adjunctive treatment option for this patient. The suggested mechanisms of action include rapid cell ingrowth and neovascularization, low immunogenicity, and bacteriostatic properties of the FSG, all of which have previously been reported.

.png)