Case Series/Study
(CS-136) Ovine Forestomach Matrix in the Surgical Management of Complex Volumetric Soft Tissue Defects: A Retrospective Case Series
Friday, April 28, 2023
7:15 PM - 8:30 PM East Coast USA Time
Michael Cormican, MD; Shane Dowling, PA-C
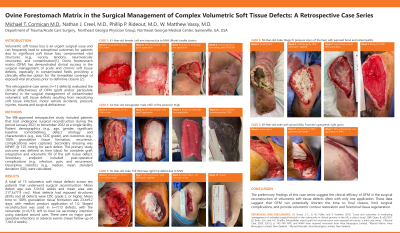
Introduction: Volumetric soft tissue loss is an urgent surgical issue and can frequently lead to suboptimal outcomes for patients due to significant soft tissue loss, compromised vital structures (e.g., viscera, tendons, neurovascular structures), and contamination [1]. Ovine forestomach matrix (OFM) has demonstrated clinical success in the surgical management of acute and chronic soft tissue defects, especially in contaminated fields providing a clinically effective option for the immediate coverage of exposed vital structures prior to definitive closure [2].
This retrospective case series (n=12 defects) evaluated the clinical effectiveness of OFM (graft* and/or particulate^ formats) in the surgical management of contaminated volumetric soft tissue defects resulting from necrotizing soft tissue infection, motor vehicle accidents, pressure injuries, trauma and surgical dehiscence.
Methods: The IRB-approved retrospective study included patients that had undergone surgical reconstruction during the period January 2021 to November 2022 at a single facility. Patient demographics (e.g., age, gender, significant baseline comorbidities), defect etiology and characteristics (e.g., size, CDC grade), and outcomes (e.g., 100% granulation tissue formation, recurrence, complications) were captured. The primary study outcome was defined as time (days) for complete graft integration and volumetric fill of the soft tissue defect. Secondary endpoint included post-operative complications (e.g., infection, pain, and recurrence). Descriptive statistics (e.g., median, mean, standard deviation (SD) were calculated.
Results: There was a total of twelve (12) volumetric soft tissue defects across ten (10) patients that underwent surgical reconstruction. The mean defect age was 3.8±5.8 weeks and mean size was 210.4±86.2 cm2. Most defects had exposed structures (83%) and all defects were CDC grade 2, or higher. The mean time to 100% granulation tissue formation was 24.1±9.3 days, with a median product application of 1.0. Staged reconstruction was used in n=7/12 defects, with the remainder (n=5/12) left to heal via secondary intention using standard wound care. There were no major post-operative complications to a mean follow-up of 6.0±1.7 weeks.
Discussion: The preliminary findings of this case series suggest the clinical efficacy of OFM in the surgical reconstruction of volumetric soft tissue defects. These data suggest that OFM can potentially shorten the time to final closure, limit surgical complications, and provide volumetric contour restoration and functional tissue regeneration.
This retrospective case series (n=12 defects) evaluated the clinical effectiveness of OFM (graft* and/or particulate^ formats) in the surgical management of contaminated volumetric soft tissue defects resulting from necrotizing soft tissue infection, motor vehicle accidents, pressure injuries, trauma and surgical dehiscence.
Methods: The IRB-approved retrospective study included patients that had undergone surgical reconstruction during the period January 2021 to November 2022 at a single facility. Patient demographics (e.g., age, gender, significant baseline comorbidities), defect etiology and characteristics (e.g., size, CDC grade), and outcomes (e.g., 100% granulation tissue formation, recurrence, complications) were captured. The primary study outcome was defined as time (days) for complete graft integration and volumetric fill of the soft tissue defect. Secondary endpoint included post-operative complications (e.g., infection, pain, and recurrence). Descriptive statistics (e.g., median, mean, standard deviation (SD) were calculated.
Results: There was a total of twelve (12) volumetric soft tissue defects across ten (10) patients that underwent surgical reconstruction. The mean defect age was 3.8±5.8 weeks and mean size was 210.4±86.2 cm2. Most defects had exposed structures (83%) and all defects were CDC grade 2, or higher. The mean time to 100% granulation tissue formation was 24.1±9.3 days, with a median product application of 1.0. Staged reconstruction was used in n=7/12 defects, with the remainder (n=5/12) left to heal via secondary intention using standard wound care. There were no major post-operative complications to a mean follow-up of 6.0±1.7 weeks.
Discussion: The preliminary findings of this case series suggest the clinical efficacy of OFM in the surgical reconstruction of volumetric soft tissue defects. These data suggest that OFM can potentially shorten the time to final closure, limit surgical complications, and provide volumetric contour restoration and functional tissue regeneration.

.png)
